Patients who suffer medical injury want to be heard
Patients who have suffered harm due to medical injury feel better when medical staff listen closely to what they have to say about the experience, a new study shows.
Patients who have suffered harm due to medical injury feel better when medical staff listen closely to what they have to say about the experience, a new study shows.
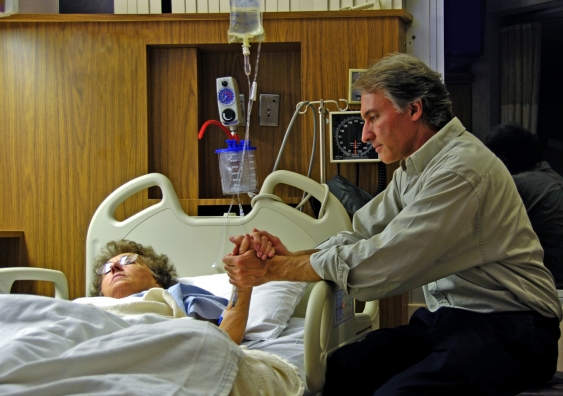
Patients who have suffered harm due to medical injury feel better when medical staff – especially the doctor who made the error – listen closely to what they have to say about the experience, a new study shows.
Patients also want to know what a hospital is doing to make sure the same mistake doesn’t happen to other patients, say authors of the report, which comes amid a growing trend among US hospitals to adopt what are known as communication-and-resolution programs (CRPs) to handle cases of medical malpractice.
The paper, Patients’ Experiences with Communication-and-Resolution Programs After Medical Injury, published in the Journal of the American Medical Association (JAMA) Internal Medicine, has major implications for Australia’s health system, says one of its authors, Dr Jennifer Moore, a senior law lecturer at UNSW Sydney.
Moore says hospitals are interested in resolving medical injuries with patients before medical malpractice claims are filed.
CRPs aim to improve patient safety and reduce liability costs by providing meaningful disclosures, apologies and pro-active compensation offers to patients rather than waiting for a patient to take legal action.
"But despite increasing interest in this approach, this was the first time that researchers were given permission to talk to US patients and family members about their experiences with CRPs," says Moore.
"We wanted to find out how patients and their families felt about hospitals’ responses after there had been a medical injury. We wanted to find out what helped and what hindered reconciliation."

Dr Jennifer Moore. Photo: Anna Kucera
Moore collaborated with Dr Marie Bismark at the University of Melbourne and Professor Michelle Mello from Stanford University. Their research included interviews with 40 patients, family members and staff at three US hospitals that operate CRPs – Stanford Medical Center, Beth Israel Deaconess Medical Center (Harvard) and Baystate Hospital.
Although 18 of 30 patient and family participants (60%) reported positive experiences with CRPs overall and continued to receive care at the hospital, they said hospitals rarely communicated information about efforts to prevent recurrences.
Most participants (35 of 40) reported it was helpful to include plaintiffs’ lawyers in these discussions because it helped build trust between families and hospitals, and because they could help assess whether compensation offers were fair.
Medical injuries are a significant cause of death around the world. A 2016 Johns Hopkins study suggests medical errors are the third-leading cause of death in US.
"There are three takeaway messages from the study’s results," says Moore. "The first is that patients need to be heard. It may mean listening for a very long time and letting the patient’s priorities lead the conversation. Second, plaintiffs’ lawyers can play an important role and help restore trust. Third, it is not enough to take action to improve things; it is really important that the patient safety efforts are communicated to the patient and family."
Listen to a podcast about the study here.