Commonly prescribed kidney medication ‘ineffective’: clinical trial
Medication prescribed to one in five chronic kidney disease patients is ineffective, a major clinical trial has found.
Medication prescribed to one in five chronic kidney disease patients is ineffective, a major clinical trial has found.
Isabelle Dubach
Media and Content Manager
+61 432 307 244
i.dubach@unsw.edu.au
Allopurinol does not prevent worsening of kidney disease – despite up to 20 per cent of kidney disease patients being prescribed the medication, results of a major clinical trial have revealed.
Researchers from UNSW and The George Institute for Global Health collaborated with researchers from the Australasian Kidney Trials Network to conduct a two-year trial – the CKD-FIX Study – across 31 hospitals in Australia and New Zealand. They enrolled 369 patients with chronic kidney disease deemed at increased risk of further progression in the trial.
The results were published today in the New England Journal of Medicine, one of the most prestigious medical journals in the world.
The researchers compared the use of allopurinol – a commonly used medication to lower blood levels of urate (also known as uric acid) – to a placebo and found it made no difference to the rate of kidney function decline.
“We found the kidney function declined at a similar rate in patients receiving allopurinol and those receiving placebo,” says study co-lead Sunil Badve, Conjoint Associate Professor at UNSW Medicine and Senior Research Fellow at The George Institute for Global Health.
“Our findings have major implications – one in five individuals with chronic kidney disease are on medication like allopurinol to lower elevated blood levels of urate. Now we know that they are likely taking medication that is of no benefit to them, unless they have other conditions that allopurinol is effective against, like gout.”
Allopurinol can have side effects, like severe allergic reactions and skin rashes. The researchers say it is important that people taking allopurinol to lower blood urate levels did not abruptly stop the treatment, but first discussed this with a doctor.
Currently available treatment options for slowing the progression of chronic kidney disease are limited and only partially effective.
“There is a huge need for new treatments for this condition,” A/Prof Badve says.
“We chose allopurinol – a medication originally developed to treat gout – for our trial because it’s a commonly prescribed to lower patients’ blood levels of urate, a waste product created by the body’s metabolism.
“High levels of urate in the blood are associated with an increased risk for chronic kidney disease – about 70-75% of people with chronic kidney disease have elevated blood levels of urate.
“However, up until our study we didn’t know if lowering blood urate levels through that medication actually slowed the process of progression of chronic kidney disease.”
A/Prof Badve says the results indicate that the widely held view that elevated blood urate levels were responsible for rapid decline of kidney function was probably wrong.
“Based on our results, it appears elevated blood urate levels are more likely an indicator of reduced kidney function, rather than a cause,” he says.
Professor Sean Emery, Senior Vice Dean - Research and Operations at UNSW Medicine, says “Independent, academic research through coordinated networks is critical to changing health outcomes. The work published today led by Professor Badve highlights the importance of using collaborative research networks to reveal important and significant new findings. In this instance we now know that a routine intervention in nephrology can no longer be justified. Clinical practice will now change globally.”
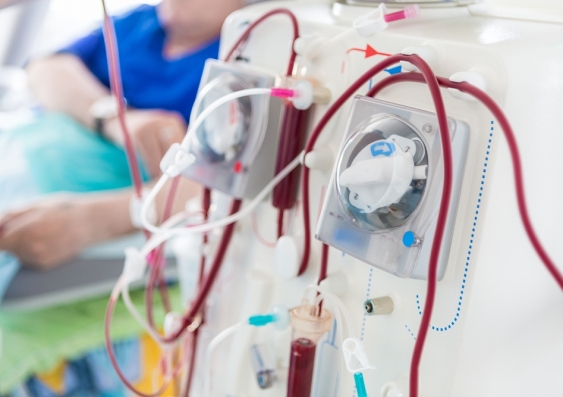
Approximately 1.7 million Australians aged 18 years and older have chronic kidney disease. Some of these people are at a higher risk of further decline in kidney function – also known as progression of chronic kidney disease – to the point of needing dialysis or kidney transplantation. More than 3,000 Australians develop kidney failure requiring dialysis each year and there are currently more than 13,000 Australians receiving dialysis.
The CKD-FIX study was sponsored by The University of Queensland and coordinated by the Australasian Kidney Trials Network. Professor David Johnson, Queensland Kidney Transplant Service Medical Director was the Chair of the Trial Steering Committee and in New Zealand, the trial was led by Dr Janak de Zoysa from the University of Auckland and Waitemata District Health Board.
The study was funded by research grants from the National Health and Medical Research Council of Australia and the Health Research Council of New Zealand and involved five investigators from UNSW: Conjoint Associate Professor Sunil Badve, Dean of Medicine Professor Vlado Perkovic, Professor Ric Day, Conjoint Associate Professor Graham Jones and Conjoint Associate Lecturer Dr Anushree Tiku. The full study is available in the New England Journal of Medicine.
Researchers compared the use of allopurinol – a commonly used medication to lower blood levels of urate (also known as uric acid) – to a placebo and found it made no difference to the rate of kidney function decline.