New research shows Aboriginal and Torres Strait Islander children are more than one and a half times more likely to be hospitalised for unintentional injuries than non-Indigenous children, prompting calls for more targeted child injury prevention programs.
The UNSW-led study is the first to investigate differences in hospitalisation rates for unintentional injury between Aboriginal and non-Aboriginal children in Australia, using linked data to follow children from birth to age 13 years.
The results suggest Aboriginal children suffer a disproportionately high burden of unintentional injury, and the gap between the two groups is wider than previously thought.
The study, led by UNSW’s Centre for Big Data Research in Health, has been published today in the American Journal of Public Health.
Hospitalisations as transport injuries and poisoning are largest in major cities and inner regional areas, which goes against the prevailing view.
Researchers analysed hospital and mortality data for more than 1.12 million children born in a NSW hospital between 2000 and 2012. Of these, 35,749 children were identified as Aboriginal.
The study found a much higher risk of injury, requiring hospitalisation, for Aboriginal children from poisoning, burns and transportation-related causes compared to non-Aboriginal children.
It found only a small difference in the risk of hospitalisation between Aboriginal and non-Aboriginal children for falls, which is the leading type of unintentional injury in all Australian children.
“Despite the national goals to reduce childhood injury and health inequalities between Aboriginal and non-Aboriginal peoples, there remains substantial inequalities in hospitalisations for unintentional injuries between these two groups,” Professor Louisa Jorm, Foundation Director of the Centre for Big Data Research in Health at UNSW, said.
The study is the first to consider and exclude factors such as rural or remote locations and socio-economic status in assessing unintentional injuries in Aboriginal children.
“Our results also indicate that these inequalities are even larger than previously reported and are not only a result of the greater proportion of Aboriginal people living in rural areas,” Professor Jorm said.
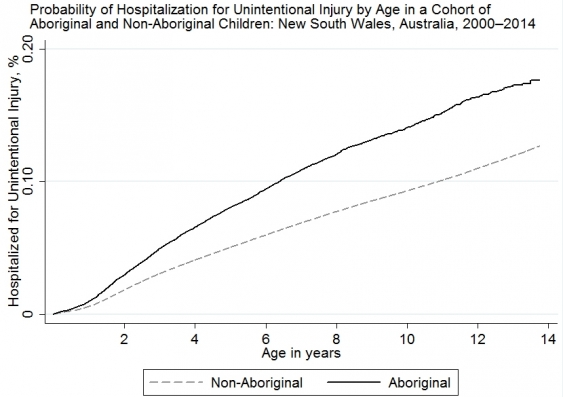
The UNSW-led study is the first to investigate differences in hospitalisation rates for unintentional injury between Aboriginal and non-Aboriginal children in Australia, using linked data to follow children from birth to age 13 years.
“We were surprised to find that the substantial inequalities in hospitalisations for some causes, such as transport injuries and poisoning, are largest in major cities and inner regional areas, which goes against the prevailing view.
“Unintentional injuries in children are highly preventable. These findings indicate that injury prevention measures that specifically address injury risks in Aboriginal children, and geographically focused interventions that target areas with high rates of child injury, have the potential to improve Aboriginal child health.
“Broad population-level prevention programs alone are unlikely to reduce these health inequalities,” Professor Jorm said.
The researchers also highlighted a lack of injury prevention programs specifically targeted at Aboriginal communities.
“With the exception of road transportation, there are few current prevention activities that specifically target Aboriginal children,” study lead author and UNSW researcher, Mr Holger Möller, said.
“We would like to see a greater investment in targeted injury prevention programs to help parents provide a safe environment for their children to grow up in,” Mr Möller said.
The study was funded by the National Health and Medical Research Council and conducted in partnership with the Australian National University, the George Institute for Global Health and the University of Wollongong.



