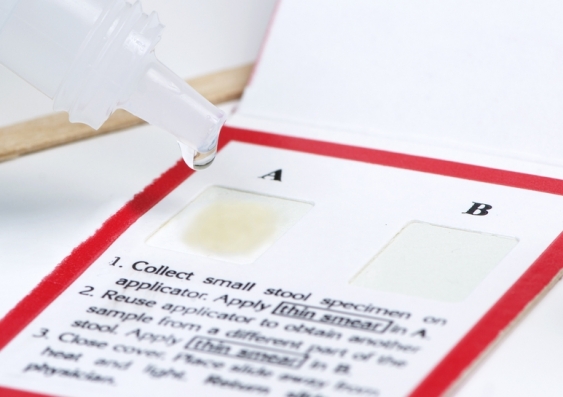
A new, Australian-first study by Cancer Council NSW has shed light on the factors that influence whether or not someone participates in bowel cancer screening. The analysis of almost 100,000 people showed that smokers, disadvantaged groups and those with non-English speaking backgrounds were among the groups less likely to access screening.
Using data from the Sax Institute’s 45 and Up Study, the study’s aim was to find out how a range of factors would influence someone’s likelihood to access bowel cancer screening, either through a program like the National Bowel Cancer Screening Program (NBCSP) or through other, more ad hoc forms of bowel screening.
The study analysed data of over 91,000 people. Over 76% reported that they had been screened for bowel cancer before. Of those study participants that were eligible for the National Bowel Cancer Screening Program, 52% reported having participated in it.
“We found that participation in the NBCSP was lowest in those living in the most socioeconomically disadvantaged areas,” said lead author Emily He, PhD student at UNSW Sydney and researcher at Cancer Council NSW.
“Also, we found that current smokers, people who did not attend screening for other cancers, those who had lower levels of education, people who did not speak English at home as well as those who self-reported poor health were less likely to have ever participated in the NBCSP.”
Cancer Council strongly encourages all Australians aged 50-74 years to take part in the NBCSP when they are sent the test kit.
“The findings underpin the need for a large-scale mass media public education campaign to increase screening participation across the whole population, including in those less likely to screen,” said Paul Grogan, Director, Public Policy and Knowledge Management at Cancer Council Australia.
“We’re also calling on the Government to revive its highly effective National Tobacco Campaign, to encourage smokers to quit. When smokers quit, their health automatically improves. For many, it’s also a time to take additional steps to improve their health. The time is right for a comprehensive cancer prevention package, to improve bowel cancer screening participation and reduce smoking prevalence – and create a win-win, where disadvantaged and high-risk groups can take greater control of their health,” Mr Grogan continued.
Professor Karen Canfell, Director of Research at Cancer Council NSW, concluded: “A previous study of ours has shown that even a modest increase in participation in the program would have an incredible impact on bowel cancer cases and deaths – so don’t be embarrassed, a simple stool check could save your life.
“Ninety per cent of bowel cancers can be cured if detected early. Finding bowel cancer early can therefore substantially improve your chance of surviving the disease.”