Healthcare for people with macular eye disease can be improved and unnecessary referrals to ophthalmologists significantly reduced through an innovative system of referral to a centre that specialises in these potentially blinding conditions, UNSW research shows.
Macular eye disease, including age-related macular degeneration, is a rising cause of blindness worldwide. These diseases of the retina lead to progressive, painless loss of central vision, affecting people’s ability to see fine detail, drive, read and recognise faces.
Optometrists are under-utilised, despite their ability to provide regular monitoring and manage cases with low risk of vision loss.
“Preventing visual loss from macular disease requires early and accurate identification and management,” says study lead author Angelica Ly, an optometrist at the Centre for Eye Health at UNSW.
“With an ageing population in Australia putting pressure on services, we need to ensure people move through the eye care system as efficiently as possible. Errors in diagnosis or delayed treatment can have profound effects on people’s daily lives, reducing their independence and doubling their risk of depression.”
Under the present two-tiered system, community optometrists who suspect patients have macular disease refer them to specialist eye doctors called ophthalmologists.
Unnecessary referrals, due to false positive diagnoses, can overburden limited ophthalmology services and lead to delays in treatment for other patients who do have the disease. The cost, travel and waiting times to see an ophthalmologist can also deter some people with disease from going for timely treatment.
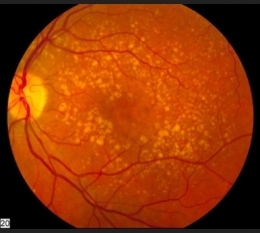
Image of the back of the eye showing age-related macular degeneration: National Eye Institute, National Institutes of Health
The UNSW team, which included Dr Lisa Nivison-Smith, Dr Michael Hennessy and Professor Michael Kalloniatis, evaluated a new, collaborative three-tier system, in which community optometrists referred patients with suspected macular disease to the Centre for Eye Health, which is a joint initiative of Guide Dogs NSW/ACT and UNSW.
The patients were assessed at the Centre by highly trained optometrists using advanced imaging equipment that detects macular disease. A study of the outcome of 291 cases referred between July 2013 and June 2014 is published in the journal Ophthalmic and Physiological Optics.
“We found that the number of cases without a clear diagnosis was halved, from 47 per cent of referrals to 23 per cent,” says Ly, a PhD candidate in the UNSW School of Optometry and Vision Science.
“As well, we found only 16 per cent of cases needed to be referred to a face-to-face consultation with an ophthalmologist. The remaining 84 per cent of cases could remain under ongoing optometric care, either with their community optometrist or by returning to the Centre for Eye Health.
“Optometrists are under-utilised, despite their ability to provide regular monitoring and manage cases with low risk of vision loss. This innovative three-tier model of care is an effective and cost-saving way to make sure people with macular disease get to see the right professionals at the right time,” she says.
Reducing false positive diagnoses and unnecessary trips to the doctor can also reduce patient’s anxiety about their eye health.
About 8.7 per cent of people worldwide have age-related macular degeneration. There are about five times as many optometrists in Australia as ophthalmologists.



